Hearing that your semen analysis shows zero sperm count can be deeply distressing. Many men immediately assume this means permanent infertility. In reality, azoospermia does not always mean that fatherhood is impossible. With proper evaluation and modern fertility treatment, many men are able to achieve biological parenthood.
This comprehensive guide explains azoospermia in detail, including its causes, types, diagnosis process, available treatment options, success expectations, and what steps you should take next.
What Is Azoospermia?
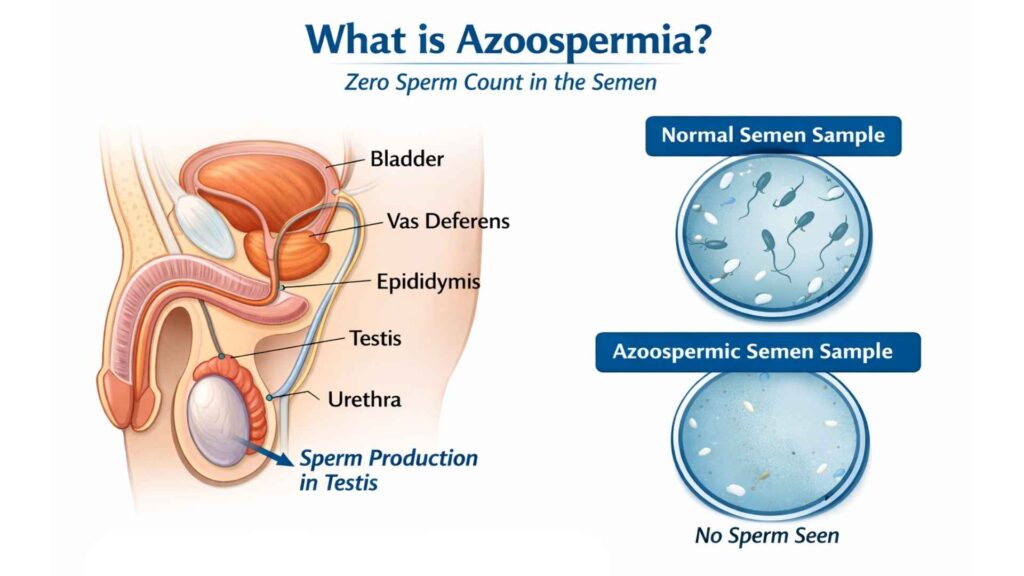
Azoospermia is a medical condition in which no sperm cells are found in the semen after laboratory examination. It affects approximately 1 percent of all men and 10 to 15 percent of men undergoing evaluation for infertility. Low sperm count is known as oligospermia, whereas the complete absence of sperm in the semen is termed azoospermia. This distinction is important because oligospermia indicates reduced sperm numbers, while azoospermia requires detailed evaluation to determine whether sperm production is impaired or if a blockage is preventing sperm from entering the semen.
Semen may appear completely normal in color, texture, and volume. The condition can only be detected through laboratory testing.
It is important to understand that azoospermia does not always mean that the body is not producing sperm. In some cases, sperm are produced but cannot reach the semen due to a blockage.
How Sperm Production Normally Works
To understand azoospermia, it helps to know how sperm are made.
Sperm production occurs inside the testes in tiny structures called seminiferous tubules. This process is controlled by hormones released from the brain, primarily:
- Follicle stimulating hormone
- Luteinizing hormone
- Testosterone
Once produced, sperm travel through the epididymis and vas deferens before mixing with seminal fluid during ejaculation.
If there is a hormonal issue, testicular production problem, or physical blockage anywhere along this pathway, azoospermia can occur.
Types of Azoospermia
Correct classification is essential because treatment depends entirely on the type.
Obstructive Azoospermia
In this condition, sperm production is normal, but a blockage prevents sperm from entering the semen.
Common causes include:
- Previous vasectomy
- Infection causing scarring
- Congenital absence of the vas deferens
- Ejaculatory duct obstruction
- Injury or surgical complications
Hormone levels are usually normal. Testicular size is typically normal as well.
Non-Obstructive Azoospermia
This occurs when sperm production is severely reduced or absent due to testicular failure or hormonal problems.
Common causes include:
- Genetic abnormalities such as Y chromosome microdeletions
- Klinefelter syndrome
- Severe varicocele
- Undescended testes in childhood
- Radiation or chemotherapy exposure
- Hormonal disorders affecting the pituitary gland
FSH levels are often elevated in these cases, indicating the testes are not responding adequately.
Causes of Azoospermia in Detail
Hormonal Imbalance
The brain regulates sperm production. If the pituitary gland does not release enough stimulating hormones, sperm production may decrease significantly.
Conditions include:
- Hypogonadotropic hypogonadism
- Pituitary tumors
- Thyroid dysfunction
- Elevated prolactin levels
These cases often respond well to hormone therapy.
Genetic Causes
Genetic testing may reveal underlying chromosomal abnormalities.
Examples include:
- Klinefelter syndrome
- Y chromosome microdeletions
- CFTR gene mutations
Genetic evaluation is important because some conditions may be passed to offspring.
Testicular Damage
Damage to the testes may result from:
- Severe infections
- Trauma
- Torsion
- Chemotherapy
- Radiation therapy
- Long term anabolic steroid use
In these cases, sperm production may be partially or completely affected.
Varicocele
A varicocele is enlargement of veins within the scrotum. Severe cases can impair sperm production by increasing scrotal temperature and oxidative stress.
Lifestyle and Environmental Factors
Although lifestyle alone rarely causes complete azoospermia, it can worsen fertility issues.
Contributing factors include:
- Smoking
- Excess alcohol use
- Obesity
- Chronic stress
- Exposure to industrial chemicals
- Excessive heat exposure
Symptoms of Azoospermia
Most men experience no physical symptoms.
Possible signs may include:
- Inability to conceive after one year of regular unprotected intercourse
- Reduced facial or body hair in hormonal cases
- Small testicles
- Low sexual desire
- History of childhood testicular problems
Often, infertility is the only noticeable symptom.
How Azoospermia Is Diagnosed
Accurate diagnosis requires a stepwise medical approach.
Step 1: Repeat Semen Analysis
At least two semen tests are performed. The sample is centrifuged to check for rare sperm.
Step 2: Hormone Blood Tests
Tests typically include:
- FSH
- LH
- Testosterone
- Prolactin
- Thyroid function
These help determine whether the issue is hormonal.
Step 3: Physical Examination
A specialist evaluates:
- Testicular size
- Presence of vas deferens
- Signs of blockage
- Varicocele detection
Step 4: Imaging Studies
Scrotal ultrasound may identify structural abnormalities.
Step 5: Genetic Testing
Recommended in non obstructive cases.
Step 6: Testicular Biopsy or Micro-TESE
In selected cases, sperm retrieval procedures are performed to look for viable sperm directly from testicular tissue.
This step is both diagnostic and therapeutic.
Treatment Options for Azoospermia
Treatment depends entirely on the cause.
Hormonal Therapy
If azoospermia is due to hormone deficiency, medications can stimulate sperm production.
Options include:
- Gonadotropin injections
- Clomiphene citrate
- hCG therapy
Improvement may take several months.
Surgical Correction of Blockage
In obstructive azoospermia, microsurgery can reconnect sperm pathways.
Procedures include:
- Vasovasostomy
- Vasoepididymostomy
- Transurethral resection of ejaculatory duct
Success depends on the duration and location of obs
truction.
Sperm Retrieval Techniques
If sperm cannot reach semen naturally, they may still be present inside the testes.
Common procedures:
- PESA
- TESA
- Micro-TESE
Micro-TESE is particularly effective in non obstructive azoospermia.
IVF with ICSI for Male Infertility
Intracytoplasmic sperm injection allows a single healthy sperm to be injected directly into an egg.
This technique has revolutionized male infertility treatment and significantly improved pregnancy rates.
In cases where sperm retrieval is successful, assisted reproductive techniques such as IVF with ICSI offer high pregnancy success rates. Choosing an experienced fertility center with expertise in male infertility management is important for better outcomes.
Donor Sperm Option
If no viable sperm are found, donor sperm may be considered after counseling.
Success Rates and Expectations
Success depends on:
- Type of azoospermia
- Age of female partner
- Quality of retrieved sperm
- Overall reproductive health
Obstructive cases generally have high sperm retrieval success. Non obstructive cases vary but still offer hope with advanced techniques.
Emotional and Psychological Considerations
Male infertility often affects confidence and emotional well being. Feelings of guilt, frustration, or anxiety are common.
Support from partners and counseling can help couples cope with the stress of diagnosis and treatment.
Remember, infertility is a medical condition, not a personal failure.
When to Seek Medical Advice

You should consult a fertility specialist if:
- Pregnancy has not occurred after one year of regular attempts
- A semen analysis shows zero sperm
- There is history of testicular injury or surgery
- Hormonal symptoms are present
Early diagnosis improves treatment planning. Early evaluation at a specialized fertility clinic can improve treatment planning and success rates.
Final Thoughts
Azoospermia is a complex but manageable condition. Zero sperm count does not automatically mean the end of biological fatherhood. With proper diagnosis, modern fertility treatments, and individualized medical care, many men achieve successful outcomes.
If you or your partner are facing male infertility, do not delay evaluation. Early medical guidance opens more options and improves overall success rates.
Medical science continues to advance, offering real hope where once there was uncertainty.
Frequently Asked Questions
Is azoospermia curable?
Some types are treatable, especially obstructive and hormone related cases.
Can lifestyle changes reverse azoospermia?
Lifestyle improvement supports fertility but may not reverse severe testicular failure.
Is azoospermia permanent?
Not always. Many men achieve biological fatherhood through advanced reproductive techniques.
Can men with azoospermia have normal sexual function?
Yes. Sexual function and sperm production are separate processes.





